Did you know that 36% of U.S. counties are considered maternity care deserts? That statistic probably worries you. You want to support vulnerable mothers, but static clinics can’t reach everyone. You are likely wondering, is a mobile pregnancy unit investment really worth the cost?
If you don’t fill this gap, moms in your area risk going without vital prenatal care. That’s a scary reality. But imagine a desired state where you bring the clinic right to their driveway or nearby community. That solves the problem and changes lives.
We have been in business for over 10 years and have manufactured more than 150 mobile medical units. We’ve helped organizations like Women’s & Infant’s Hospital, CalOptima, and Siskiyou County reach their goals. AVAN Mobility is trusted by healthcare networks across the U.S. to deliver innovative vehicle solutions that remove barriers to healthcare.
You need to know if a pregnancy mobile unit fits your budget and mission. Here is what we’ll cover in this article:
- The real costs involved.
- The value it brings to your community.
- If a mobile OB-GYN setup is the right move for you.
Is a mobile pregnancy unit worth the price tag?
You can expect to pay between $170,000 to $290,000 for a mobile pregnancy unit. That range probably makes you pause. It feels big. It also feels vague. The reason it stretches like that is simple. Every program is different. Some OB-GYN teams can work well with a lean setup. Others require a comprehensive “doctor’s office on wheels” with portable equipment, technology, and comfort features that support mobile care for many years.
So the real question in your mind is less “What does it cost?” and more “Is this worth it for us?”
In many parts of the U.S., the gap in maternity care is growing. Over 35% of counties are now maternity care deserts, with no local OB-GYN or birthing facility. That affects about 2.3 million women of childbearing age and 150,000 births each year.
Rural areas feel this even more. Nearly half of rural counties have no local maternity care at all. You see that gap in real life, not in a chart. You see missed visits, risky late care, and families who feel like the system forgot them.
A mobile pregnancy unit gives you a way to close that gap instead of working around it.
How can a mobile pregnancy unit change life in your area?
Picture a small county in rural Mississippi. The local hospital closed its labor and delivery unit a few years ago. Now, pregnant patients drive two or more hours for routine care. Many people skip visits when money, gas, or childcare is scarce. The state has some of the highest infant death and preterm birth rates in the country, and leaders have even declared public health emergencies around infant deaths.
Now imagine that same county with a pregnancy mobile unit that parks:
- At the high school, one week
- At a church parking lot, the next
- Outside a community center on Saturdays
Moms get blood pressure checked closer to home. Teens get early prenatal care in a familiar place. High-risk patients are seen before problems escalate.
Or think about a Tribal health team in northern Arizona. Patients may drive on two-lane highways or dirt roads for hours. Snow, heat, and work schedules all play a role. A mobile OB-GYN van that follows a set route across the region gives them something solid to count on. Same nurse faces, same calendar, and same support.
When you weigh the price of a mobile pregnancy unit, this is what you measure it against. You are not comparing it to a van.
You are comparing it to:
- Late prenatal care
- Emergency transports
- Burned-out staff
- Families losing trust in the system
What are you really paying for with a mobile pregnancy unit?
The cost of a pregnancy mobile unit is tied to how much care you want to deliver safely and comfortably on the road. In this section, you’ll learn about some of the things that shape the price.
Doctor’s office on wheels setup:

You are paying for a layout that works like a small clinic room. There is space to talk, examine, chart, and move without bumping into everything.
Floor-to-ceiling cabinetry:

Cabinets keep supplies, charts, and equipment organized and off the floor. Good storage keeps visits smoother and protects gear.
Patient bed with under-bed storage:

The bed needs to feel safe and steady, with room under it for items for your staff and patients.
Options for sink and fridge:

A sink supports basic hygiene tasks. A small medical-grade fridge can hold certain medication or samples, if your program needs that.
Power supply:

The van needs a smart power system that runs lights, devices, and some medical equipment. This can include inverters, batteries, and shore power.
Rear heat and air conditioning options:

Patients and staff should feel comfortable in both Texas heat and Montana winters. Climate control in the rear matters a lot.
Clean, comfortable environment:

Floors, walls, and finishes should be easy to wipe and keep fresh. A calm space helps people relax during visits.
Conventional outlets, 12V plugs, and USB ports:

You need enough places to plug in laptops, printers, chargers, and any small devices used during care.
Diagnostic set:
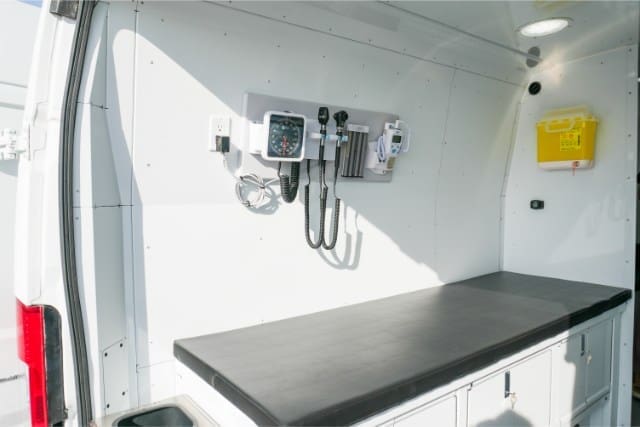
Basic diagnostic tools, such as an otoscope and an ophthalmoscope, support everyday checks and screening.
Awning:

An awning can create shaded space outside for intake, education, or a small waiting zone during busy events.
Privacy curtain:

This small detail builds dignity. A curtain gives patients a sense of safety during exams or while changing.
Medical equipment:
From blood pressure cuffs and fetal Dopplers to ultrasound machines, your list here shapes both care and cost.
You pick from these options based on what your patients face and what your staff need to work safely and calmly.
How can a mobile pregnancy unit create a positive financial impact for your program?
When you bring prenatal care closer to the people you serve, your numbers begin to shift in ways that are both human and financial. A mobile pregnancy unit can help stabilize your budget over time because steady prenatal care reduces costly emergencies, late care complications, and preventable hospital use.
Across the country, rural communities face higher pregnancy-related risks because of long travel distances and fewer OB-GYN providers. Research shows that about 2.2 million women of childbearing age live in rural counties with limited access to maternity care. These counties also show higher rates of maternal vulnerability, which link directly to higher medical costs for both mothers and newborns.
When regular care becomes easier to access through a mobile pregnancy unit, you often see financial gains in four core areas.
Financial gains from a mobile pregnancy unit
1. Fewer missed visits: Missed prenatal appointments lead to costlier care later. According to a 1992 study, newborn and postpartum costs starting within 60 days after birth were $347 lower for pregnancies with adequate prenatal care compared with those with inadequate care.. Bringing care into the community helps families attend visits, which lowers the chance of costly complications.
2. Earlier prenatal starts: Early prenatal care reduces the risk of preterm birth. Preterm births cost the U.S. healthcare system over $26 billion every year, with one preterm birth costing an average of $65,000. Catching issues early changes both outcomes and financial strain on your program.
3. Lower emergency use: When high blood pressure, gestational diabetes, and fetal concerns are found early, the chance of a last-minute emergency drops. Emergency pregnancy care is expensive, and avoiding even a handful of urgent transfers each year can offset a large share of your program costs.
4. Better staff efficiency: A mobile OB-GYN route lets your team serve several small communities in one day, which stretches staffing dollars further. Instead of running outreach events with limited tools, your team brings a fully equipped unit that supports safer and more efficient work.
A simple example of the financial shift
Let’s take a look at an example of West Texas FQHC
A program invests $220,000 into a mobile pregnancy unit. The van runs three days a week across four small towns.
After one year, the clinic sees:
- Higher attendance at prenatal visits.
- More patients starting care in the first trimester.
- Fewer emergency transfers.
- Fewer high-cost complications.
- Better staff coverage across long distances.
Let’s attach numbers to this.
If the unit prevents even:
- 3 preterm births in a year, which can save around $195,000 in related care costs.
- 5 emergency transfers, which can cost up to $8,000 each, that’s another $40,000 protected.
- 20 missed prenatal visits turning into risky late care, you reduce the chance of NICU stays, which average $3,000 to $5,000 per day.
This means a single mobile pregnancy unit can protect hundreds of thousands of dollars in potential downstream spending, even while you continue paying for fuel, staff, insurance, and upkeep.
You support better health, but you also reduce avoidable expenses that strain budgets.
How do you decide if a mobile pregnancy unit is worth it for your community?
The price tag alone will never answer this for you. To decide if a mobile pregnancy unit is worth it, focus on your gaps.
Ask your team questions like:
- How far do people travel now for prenatal care?
- How many visits are missed because of transport or child care problems?
- Do you see late entry to prenatal care in your data?
- Are there towns or neighborhoods with no local OB-GYN presence?
- Are staff feeling stretched trying to cover outreach with limited tools?
You can even sketch two simple pictures:
- Today’s picture: Missed visits, travel issues, staff strain, and health risks.
- Future picture: A pregnancy mobile unit on a route, steady visits, and earlier support.
If the gap between those two pictures feels large, a mobile pregnancy unit often starts to look less like a cost and more like a key part of your care model.
Where does this leave you in deciding on this investment?
A mobile pregnancy unit in the $170,000 to $290,000 range is a serious capital decision. It should be. You’re making a choice that will shape care in your area for years to come.
When you step back, remember that you’re not just paying for cabinets and outlets.
You’re paying for:
- Safer pregnancies in places with long roads and few clinics
- Trust with families who feel left behind
- Easier workdays for staff who want to help more people in less time
For some organizations, the numbers, the gaps, and the mission all point in the same direction. For others, the timing or funding may still be in motion. Our role at AVAN Mobility is to help you see the full picture with clear eyes so you can decide if this investment fits your community and your goals.
Ready to take the next step toward stronger healthcare?
You came to this article because you’re trying to close a gap that keeps families in your community at risk. Maybe you see people facing travel barriers, missed prenatal visits, and the rising cost of late care. You wanted a clear answer about the mobile pregnancy unit investment and what it could mean for the people you serve today and in the future.
Here’s a quick look at what you learned:
- Cost range: What drives the price of a pregnancy mobile unit.
- Impact: How early care, better attendance, and fewer emergencies can protect budgets.
- Value: Why this investment can move your program from reactive care to proactive support.
Our team at AVAN Mobility has spent more than a decade helping health programs like yours turn ideas into real, working mobile medical units that reach families with dignity and care. We’ve built units for communities facing long distances, closed clinics, and growing healthcare needs, and we’ve seen what happens when a reliable mobile option finally shows up.
We stay close to our partners through planning, design, and real-world deployment, and that’s a big part of why leaders trust us across the country. If you have questions about next steps, click the button below to talk to a mobility expert. We’re here to help you move forward with clarity and confidence.
If you’re not ready to talk to a mobility expert yet, here are a few helpful resources to keep learning:
Recommended next reads
1. Mobile OBGYN vs. traditional pregnancy centers: A strong next step because it helps you compare mobile prenatal care to traditional care models so you can decide which approach fits your community best.
2. The dollars and sense of mobile medical vehicle investments: Perfect follow-up if you want another clear breakdown of long-term value and financial return.
3. Buying a mobile medical van: Your process with AVAN Mobility: This walks you step by step through what it’s like to move from interest to purchase, giving you a clear picture of what working with our team actually looks like.





