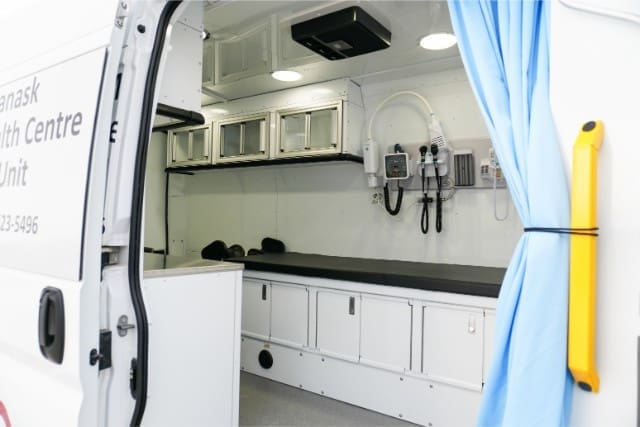
Safety incidents in a mobile clinic can feel like the “what if” you can’t shake. And you’re not being dramatic. Healthcare workers face real risks from violence. In fact, the U.S. Bureau of Labor Statistics reports that healthcare workers made up 73% of all nonfatal workplace injuries due to violence in one recent data set.
Now picture your team in a mobile clinic parked outside a shelter in Los Angeles, at a rural site in West Texas, or in a small town in Appalachia. You’re there to help. But your staff is also out there, away from hospital security, with unknown foot traffic, and sometimes patients who are scared, upset, or unpredictable. That gap between your mission and your risk can keep you up at night. You want healthcare to feel safe, calm, and dignified for everyone. You also want your team to go home in one piece.
At AVAN Mobility, we’ve spent over 10 years building 180+ mobile medical units designed to remove barriers to healthcare and help save lives. We’ve supported organizations like CalOptima and Pacific Clinics, and we hold Ford Pro Upfitter and Stellantis QPro certifications. We’re proud of that experience, and we also know there are other solid manufacturers out there, so we’ll keep this practical and buyer-friendly.
In this article, you’ll learn:
- What safety risks show up most often in a mobile clinic
- How mobile clinic safety features can lower risk
What safety incidents in a mobile clinic show up most often in the real world?
When people talk about safety incidents in a mobile clinic, they often picture one dramatic event. Real life looks different. Most safety issues build slowly. They come from the environment, unpredictability, and the simple truth that your team works outside the controlled setting of a traditional facility.
One day, your staff might be out in a corn field in Arizona providing outreach care. The next day, they could be parked downtown near a shelter in Chicago or Los Angeles, where activity never slows down. The setting changes fast. The risks change with it.
This creates a real gap for healthcare organizations. You want to reach more people. You also want your team to feel safe while doing it. Understanding the risks that show up most often is the first step toward preventing safety incidents in a mobile clinic before they happen.
Let’s break down the risks your team is most likely to face.
Unpredictable patient behaviors
Healthcare workers see people at their hardest moments. In a mobile clinic, that pressure can feel stronger because the space is smaller and more personal.
Patients may arrive stressed, scared, or overwhelmed. Some are dealing with mental health challenges. Others may be frustrated after long waits or difficult life situations. According to the CDC, healthcare workers face higher rates of workplace violence than many other professions.
Common situations include:
- Escalated conversations: A small disagreement can grow quickly in a compact space.
- Emotional overload: High stress may lead to sudden reactions.
- Limited personal space: Staff and patients are often working close together.
When you think about safety in a mobile clinic, this human factor is often the biggest concern. The goal is to create an environment where situations stay calm before they become incidents.
Location

A stationary clinic operates in one known environment. A mobile clinic works in many.
You might serve rural communities in New Mexico where help is far away. Then you move into a busy urban neighborhood in New York or Seattle, where there’s constant foot traffic. Each location introduces a new layer of risk.
Rural or remote settings often include:
- Long law enforcement response times
- Limited cell service
- Extreme weather exposure
- Challenging terrain or road conditions
Urban environments often include:
- Higher volume of walk-ups
- More unpredictable public interaction
- Noise and distractions that make situations harder to read
This constant change is a major reason safety incidents in a mobile clinic can catch organizations off guard. Yesterday’s setup might feel safe. Today’s situation could be very different.
Working alone
Inside a hospital or clinic, support is close by. In a mobile clinic, teams are often small. Sometimes there’s only one or two staff members on site.
That isolation increases pressure when something feels off.
Risks linked to isolation include:
- Delayed support when help is needed
- Limited witnesses during tense situations
- Difficulty communicating quickly under stress
Imagine a provider alone in a rural area or parked in a quiet lot after dark. Nothing may go wrong, but the lack of backup adds risk. This is a common gap organizations notice once they move from planning to real-world operations.
Environmental conditions
Safety isn’t always about people. Sometimes the environment itself becomes the risk.
Your team could face intense heat in Arizona or Texas one week, then freezing temperatures in the Midwest the next. Weather and terrain affect both staff well-being and patient safety.
Environmental risks often include:
- Heat exhaustion during hot-weather outreach
- Freezing conditions and ice hazards
- Slippery surfaces near the vehicle
- Remote roads that create access challenges
When staff are uncomfortable or fatigued, decision-making gets harder. Small issues can turn into larger safety problems faster than you expect.
Operational gaps
Sometimes the biggest risk comes from missing structure rather than from external threats.
Mobile programs often grow quickly because the need is urgent. When that happens, safety protocols can lag behind daily operations. Staff may rely on assumptions instead of clear plans.
Common operational gaps include:
- No clear plan for sharing travel locations
- Inconsistent check-ins during the day
- Unclear emergency steps
- No defined exit strategy during tense moments
These situations don’t happen because teams don’t care. They happen because mobile healthcare moves fast. Without consistent safety processes, small mistakes can stack up.
Why is understanding the risks the first step to improving safety in a mobile clinic?
Most safety incidents in a mobile clinic don’t come from one single problem. They happen when multiple factors line up at the same time.
- A stressful interaction
- A remote location
- No quick way to get support
- Unclear communication
When those gaps overlap, risk increases.
The good news is that understanding these risks changes how you plan. Once you can see where incidents start, you can build stronger systems to prevent them. That’s where the shift happens. Staff feel supported, patients feel safer, and your mission becomes easier to deliver.
Next, we’ll look at the mobile clinic safety features and practical strategies that help close these gaps and prevent safety incidents before they begin.
What mobile clinic safety features and considerations help prevent safety incidents in a mobile clinic?
Once you understand where safety incidents in a mobile clinic come from, the next step is simple. You close the gaps with practical safety features and clear operating habits. The goal is calm care delivery. When your team feels protected, they focus better, connect better, and provide stronger care.
Below are the most important mobile clinic safety features and considerations that help organizations reduce risk and feel more confident in the field.
Surveillance and safety cameras

Visible cameras play a powerful role in safety in a mobile clinic. Their biggest strength is deterrence.
When patients or visitors see cameras, it sends a clear signal that the space is monitored. That alone can discourage unsafe behavior before it starts. Most people naturally adjust when they know actions are being recorded.
How cameras help your team feel safer:
- Visibility: Staff know there is a record of what happens inside and around the unit.
- Behavior awareness: People tend to stay calmer when they realize they are on camera.
- Peace of mind: Team members feel less alone when activity is monitored.
Think about a busy outreach day near a shelter in Denver or Seattle. Foot traffic is high, emotions can be unpredictable, and your staff may feel exposed. Cameras add a quiet layer of protection that keeps the environment more controlled without changing how care feels to patients.
Panic button with law enforcement dispatch
A panic button is one of the most straightforward safety upgrades you can add to a mobile clinic.
It gives staff a fast way to call for help without reaching for a phone or speaking. If an interaction escalates, pressing one button sends an emergency alert that supports dispatching law enforcement or security.
Why this matters in real situations:
- Speed: Staff react instantly instead of fumbling with devices.
- Discretion: A button press is less noticeable during tense moments.
- Support: Help can be sent even if the staff cannot safely talk.
Picture a provider in a counseling session where emotions suddenly rise. A panic button removes hesitation. Your team knows help can be requested quietly and quickly, which lowers stress even before an incident occurs.
That calm feeling often prevents situations from escalating further.
Live feed integration to a fixed clinic
Live video connectivity can take safety to another level. A mobile clinic can be linked to a fixed clinic where team members monitor a real-time video feed from inside the vehicle.
For this setup, the unit would need customization with a Starlink package to maintain reliable connectivity, especially when operating in rural or remote regions.
Benefits of live feed monitoring:
- Real-time awareness: Off-site staff can see what’s happening immediately.
- Faster decision making: Teams back at the clinic can coordinate responses quickly.
- Shared responsibility: Field staff know they are supported even from miles away.
Imagine your team running outreach in rural Montana, where law enforcement response might take time. Remote monitoring allows staff back at your main clinic to evaluate the situation and guide next steps without delay.
This helps your organization feel connected, even when the vehicle is far from home.
Egress considerations

Egress sounds technical, but the idea is simple. It means knowing how to exit safely if a situation changes fast.
Clear exit planning is one of the most practical ways to improve safety in a mobile clinic. If staff know where and how to leave quickly, they feel more confident handling difficult moments.
Egress planning includes:
- Clear pathways: Avoid blocked exits or crowded layouts.
- Staff awareness: Everyone knows the fastest exit route.
- Planning ahead: Thinking through “what if” scenarios before they happen.
In small mobile environments, space matters. Planning exits ahead of time removes panic and creates calm decision-making when stress levels rise.
Recovery and assistance equipment
Safety isn’t always about people. Sometimes it’s about the vehicle itself.
Recovery equipment, like a winch, can help when a mobile clinic gets stuck in challenging terrain. Rural outreach often means dirt roads, snowy parking lots, or soft ground. The Trail Edition upgrade can also give your vehicle a nice boost for more challenging conditions.
How this supports safety:
- Reduces isolation: Staff aren’t stranded waiting for help.
- Protects schedules: Delays and unexpected weather exposure are reduced.
- Improves confidence: Teams feel prepared for remote environments.
Think about serving a farming community after heavy rain or traveling to a rural event site in the Southwest. Recovery tools reduce risk and keep outreach programs moving safely.
Travel plan communication
One of the most overlooked safety tools is communication.
Before heading out, staff should share travel plans and locations with a designated contact. Someone should always know where the unit is going and when it’s expected back.
Simple communication habits include:
- Location updates: Share route and destination.
- Expected timelines: Let others know when to check in.
- Point of contact: Assign one person who tracks movements.
This practice closes a major operational gap. If something unexpected happens, support teams already know where to start looking.
Regular safety check-ins
Scheduled check-ins are small habits that make a big difference.
Touch points every one to four hours allow leadership or support staff to confirm that everything is okay. They also give field teams a chance to flag concerns early.
Benefits of check-ins:
- Early problem detection: Small concerns get addressed before growing.
- Emotional support: Staff feel connected and supported.
- Routine stability: Consistency lowers stress during long outreach days.
When you’re parked miles from the nearest facility, even a quick check-in message can remind staff they are part of a larger team.
Environmental safety awareness

Safety risks go beyond patient interactions. Heat, cold, and weather conditions often impact teams more than people realize.
Your mobile clinic may operate in extreme heat in Arizona or freezing temperatures in Minnesota. These conditions affect energy levels, judgment, and physical safety.
Environmental awareness includes:
- Monitoring weather conditions before deployment
- Planning for heat or cold exposure
- Preparing for terrain or road challenges
Paying attention to environmental risk helps prevent accidents that have nothing to do with patient care but still impact your team’s well-being. Ask us about the high-capacity HVAC system you can get with our mobile clinics.
Standard operating procedures
Strong safety features work best when paired with clear processes. That’s where standard operating procedures come in.
SOPs turn safety from a reaction into a routine. They help teams know exactly what to do without guessing.
Effective safety SOPs often include:
- Pre-deployment checklists
- Communication expectations
- Emergency response steps
- Check-in schedules
- Exit planning
When everyone follows the same playbook, stress goes down. Staff spend less time wondering what to do and more time focused on patients.
How does combining mobile clinic safety features create a calmer care environment?
No single tool prevents all safety incidents in a mobile clinic. The real strength comes from combining features and habits together.
- Cameras discourage problems
- Panic buttons speed up support
- Live feeds connect your team to backup
- Clear SOPs create consistency
When these pieces work together, the entire environment changes. Staff feel safer. Patients sense calm. Care becomes more human and more focused.
And that’s the real goal. A mobile clinic should feel like a safe, welcoming place for everyone inside. When your team feels confident, they can focus on what they came to do in the first place. Serve people, remove barriers, and help communities heal.
Got any questions about mobile clinic safety?

You came here because safety incidents in a mobile clinic feel like the one risk that can undo all the good you’re trying to do. You want to reach people in hard places, but you also want your staff to feel safe and steady while they provide care.
What you learned in this article:
- Risks: Safety incidents in a mobile clinic often come from unpredictable behavior, changing locations, isolation, weather, and weak routines.
- Solutions: Mobile clinic safety features and simple team habits can lower stress, reduce risk, and help care feel calmer for everyone.
At AVAN Mobility, we put a lot of effort into helping you make smart decisions before you buy. That’s why we publish straightforward, buyer-first resources in our Learning Center and share guidance to help you plan with confidence. We’ve been building mobile medical units for over 10 years, and our work stays focused on removing barriers to care and supporting programs across the U.S. If you’ve got questions about safety in a mobile clinic, click the button below to talk to a mobility expert. We’ll help you think it through like a partner, not a pitch.
If you’re not ready to talk to a mobility expert yet, we have a few other resources you should check out to learn more.
Recommended next reads
- Mobile medical van customization: What is it all about? This article helps you understand how custom layouts and features can directly support safety, workflow, and staff confidence in daily operations.
- Top 5 tips on how to start a mobile medical clinic: If you’re early in planning, this gives you a practical overview of the steps, decisions, and preparation needed to launch successfully.
- How much does a mobile clinic cost? We break down the cost range you can expect to pay for a mobile clinic.