Have you ever watched someone’s health spiral because they couldn’t get to a clinic in time? It’s heartbreaking. Across the U.S., 133 million people live with at least one chronic disease. Many of those cases could have been prevented with earlier care. That’s what proactive health is all about: Getting ahead of problems before they grow.
But when people live hours from the nearest provider or can’t afford to miss work, that kind of care feels out of reach. If you’re running a community program or health organization, you’ve likely seen this gap firsthand. You want to help, but logistics, staffing, and distance keep getting in the way.
I’m Russ Evans from AVAN Mobility. I’ve worked with healthcare teams like yours across the country, who face the same challenges. My background in emergency response opened my eyes to how many lives could be saved if care reached people sooner. I believe healthcare shouldn’t start at the ER doors; it should start where people live.
That’s why our mission is simple: Build vehicles that remove barriers and save lives. And while we’re one of many in this space, what matters most to me is helping you see how mobile healthcare units can change the story for your community.
In this article, you’ll learn:
- How mobile healthcare units close care gaps before issues become crises
- Why proactive health programs work for communities and budgets
Let’s look at how we can make proactive health possible, together.
How do mobile healthcare units close healthcare gaps before issues become crises?
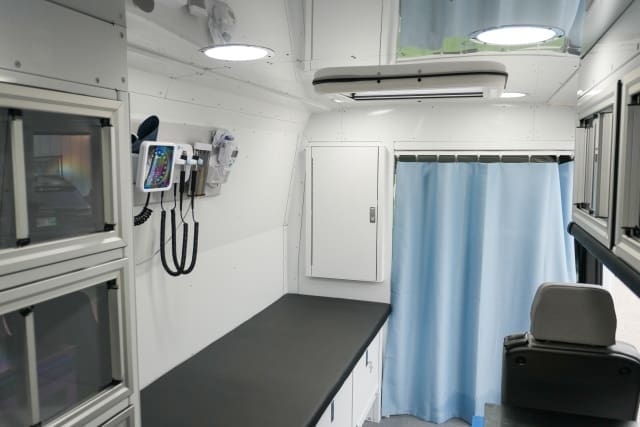
When I talk about proactive health, I’m really talking about getting ahead of problems before they snowball. Across the U.S., so many people still fall through the cracks. In some places, the nearest clinic can be 60 or even 100 miles away. Some people in small towns skip checkups for years because taking a day off work or finding a ride just isn’t possible. By the time they finally see a doctor, that simple blood pressure concern has turned into something life-threatening.
That’s where mobile healthcare units come in. They close that distance, literally. Instead of asking people to find their way to care, you bring care to them. I’ve seen organizations all over the country use mobile units to reach rural areas, tribal lands, and city neighborhoods where transportation is tough.
In West Texas, some programs use mobile mammography vans to reach women who haven’t had access to regular screenings. In North Dakota, health departments use mobile units for preventive checkups and vaccinations. The results? More people seen early, fewer emergencies later.
Here’s why it works:
- Access matters: When care comes to your doorstep, people show up.
- Trust builds: Seeing the same nurses and staff each visit helps people feel comfortable opening up.
- Problems shrink: Early screenings for things like high blood pressure or diabetes catch issues before they get out of control.
- Partnership grows: These units often work alongside local hospitals or clinics, extending care instead of competing with it.
To paint the picture, let’s talk about a few hypothetical examples that mirror what I’ve seen over the years.
Example 1: A community health team in Mississippi uses a mobile unit to visit small towns each week. Folks who’ve avoided the clinic for years start coming by for checkups. One man finds out he has early-stage diabetes and starts treatment right away instead of learning the hard way in an ER.
Example 2: A mobile clinic in Arizona parks outside a community center every other Thursday. People stop in for blood pressure checks and leave with referrals for follow-up care through telehealth. It’s simple, but it works.
These kinds of efforts make proactive health real. It’s healthcare that doesn’t wait until something’s wrong; it shows up before things go south.
I’ve always believed care should meet people where they are. Mobile healthcare units do exactly that. They make it easier for communities to take control of their health and stay out of emergency rooms that are already stretched thin.
Next, let’s look at how proactive health programs like these can actually save organizations money while improving outcomes for the people they serve.
How does proactive health cut costs and strengthen outcomes?

Proactive health pays off when you stop chasing emergencies and start catching problems early. I’ve helped teams do this for years. When care shows up on time, people skip fewer visits, use ERs less, and stay on track with screenings. That is good for your community and your budget. Mobile healthcare units make proactive health possible week after week.
Here’s the simple math. Unnecessary emergency room visits can quickly drain dollars. In 2021, treat-and-release ER visits averaged about $750 each, adding up to $80.3 billion nationwide. Every avoidable visit you prevent keeps care dollars working closer to home. Mobile clinics help you shift those visits to primary and preventive care.
Return on investment matters to boards and funders. The Harvard-led Mobile Health Map estimates an average of $18 returned for every $1 invested in mobile clinics. That ROI comes from avoided ER visits, better chronic disease control, and quality-of-life gains. These are real programs reporting real outcomes across the U.S.
Chronic disease drives most health spending in America. The CDC reports that about 90% of national health costs go to people living with chronic and mental health conditions. Proactive health and wellness meet those conditions early with blood pressure checks, A1C tests, refills, and quick follow-ups. When a mobile team catches a trend early, you avoid a crisis later.
What moves the needle with mobile units?
- Right place: Park at schools, tribal centers, worksites, food banks, or churches so people can walk to care.
- Right cadence: Set a repeating route so folks know you’ll be back in two weeks. Trust grows with routine.
- Right mix: Offer screenings, vaccines, labs, and quick primary care visits. Close loops with referrals.
- Right follow-up: Blend mobile visits with telehealth check-ins to cut no-shows and keep momentum.
Early screening saves lives and costs. USPSTF guidance supports screening that finds disease sooner, like mammography starting at age 40 and annual low-dose CT for lung cancer for qualifying adults. A mobile unit can bring these services to people who rarely reach fixed sites. Earlier detection means less intensive treatment and better odds.
Health centers prove the model. HRSA shows patients tied into primary and preventive care use fewer expensive options like ERs and inpatient stays. Mobile programs that partner with FQHCs and hospitals extend that effect into neighborhoods and rural roads. Together, they lower the cost per patient and lift satisfaction.
You may ask how this looks in day-to-day operations. Here are hypothetical scenarios that reflect similarly to what I’ve seen leaders build:
- Great Plains loop: A county team runs a Tuesday route through three towns. Nurses do BP checks, A1C tests, and medication counseling. Over a season, fewer hypertensive spikes hit the ER. Primary care visits rise in partner clinics because referrals stick.
- Gulf Coast hub: A mobile unit parks outside a community center every other Thursday for women’s health. Mammography and follow-ups are linked to a regional hospital. More screens happen on time. Fewer late-stage surprises appear in the OR.
- Southwest tribal route: A compact unit offers vaccinations, cholesterol checks, and telehealth follow-ups. Missed appointments fall because care is local and simple to reach. People stay connected to treatment plans.
How does proactive health show up on your balance sheet?
When people think about mobile healthcare, they often picture outreach and compassion, which are absolutely part of it. But I’ll be honest: finance teams and funders also want to know if it makes sense on paper. And it does.
Let’s look at some numbers.
The average emergency room visit in the U.S. costs about $750 when it doesn’t lead to admission. If your mobile program prevents even 20 unnecessary ER visits a month, that’s $15,000 saved. Stretch that over a year, and you’ve freed up $180,000 that can go back into care delivery, staffing, or vehicle maintenance.
Now, take chronic disease. As we mentioned earlier, about 90% of healthcare spending, roughly $4.1 trillion annually, goes to managing chronic and mental health conditions. If proactive health programs reduce those incidents by even 1%, that’s a potential savings of $41 billion nationwide. You don’t need to be a giant system to see the benefit. For a community program running on a $2 million annual budget, that same 1% improvement equates to about $20,000 in avoided downstream costs.
Then there’s the ROI of mobile clinics themselves. The Mobile Health Map study that we also talked about earlier found that for every $1 invested, mobile healthcare programs return $12 to $18 in combined savings from avoided ER visits, reduced readmissions, and improved long-term health. For example, a mobile unit operating at $400,000 per year could yield $4.8 million to $7.2 million in indirect community savings.
Here’s a simplified way to visualize it:
| Category | Traditional cost (per patient/year) | Mobile medical unit intervention cost | Potential annual savings |
| ER visit (non-admit) | $750 | $0 (diverted to mobile checkup) | $750 saved per patient |
| Diabetes complication (hospitalization) | $17,500 | $200 (mobile screening) | $17,300 saved |
| Missed workdays from unmanaged chronic illness | $1,300 | $0 (prevented through ongoing care) | $1,300 saved |
| Preventive screenings | $250 | $150 (mobile-based) | $100 saved per screening plus early detection value |
Even if you ran a modest mobile program serving 2,000 patients per year, these savings add up fast.
Let’s say:
- 400 avoided ER visits = $300,000 saved
- 30 avoided diabetes hospitalizations = $519,000 saved
- 100 improved chronic care cases = $130,000 saved in productivity
That’s nearly $950,000 in total annual savings, more than twice the operating cost of many single mobile units.
What’s more, proactive health doesn’t only reduce direct costs; it stabilizes long-term budgets. When communities stay healthier, insurance claims drop, turnover decreases, and emergency contracts shrink. The ripple effect of consistent care is measurable.
In short, proactive health programs do a lot more than just close care gaps; they strengthen your financial foundation. Every early checkup, every avoided ER visit, and every managed chronic case shows up as a win on your balance sheet.
Got any questions about mobile healthcare?
You came here because you’ve seen what happens when people wait too long for care. You wanted to find real solutions that make healthcare proactive instead of reactive—and now you have a clearer path forward.
Here’s what you learned:
- Why proactive health matters: Reaching people early saves lives, time, and money.
- How mobile healthcare units help: They close access gaps and turn preventive care into everyday care.
- What the results look like: Healthier communities, fewer emergencies, and stronger financial outcomes.
At AVAN Mobility, we’ve spent over a decade helping hospitals, health centers, and outreach teams bring proactive healthcare to life. Our vehicles are designed to solve real-world challenges; from serving tribal communities in remote regions to supporting city outreach teams on tight budgets.
Every build is shaped by one goal: To save lives by removing barriers to care. That’s what makes us more than a manufacturer; we’re partners in your mission to make healthcare accessible to everyone. If you have questions, click the button below to talk to one of our mobility experts.
If you’re not ready to connect yet, here are a few helpful reads to guide your next steps:
- How much does a mobile medical unit cost in the U.S.? Understand the cost factors so you can plan your project with confidence.
- How to choose a mobile medical van: Learn more about how to choose the right mobile medical unit for your program.
- A guide to securing grants for mobile health clinics in the U.S.: Find out how programs like yours are getting funded.
These articles will help you move from understanding how mobile healthcare works to building the right plan for your own proactive health initiative.