Did you know that more than 1 in 10 adults in Georgia live with diabetes, and many more are at risk? According to the Centers for Disease Control and Prevention, diabetes continues to hit rural and underserved communities the hardest, especially across South Georgia and areas far from major care hubs like Atlanta, Macon, and Albany. Georgia’s diabetes care shortage leaves many healthcare organizations asking the same question: how do you reach patients who cannot easily reach you?
If you’re trying to close care gaps, you already feel the pressure. Missed appointments, delayed screenings, long travel times, and limited provider access create real risks for patients and real strain for your team. A mobile clinic can help bridge that gap by bringing mobile healthcare directly into the communities that need faster access to diabetes support, screenings, and follow-up care.
Our team at AVAN Mobility has spent over 10 years helping organizations like yours and the Community Clinic of Southwest Missouri remove barriers to healthcare through mobile medical units built for real community impact. We hold Ford Pro Upfitter certification and Stellantis QPro certification, and we’ve worked with healthcare teams across North America. We know we’re not the only manufacturer, and buyers deserve clear answers.
In this article, you’ll learn:
- What Georgia’s diabetes care shortage looks like today
- How mobile clinics help close diabetes care gaps
- Where a mobile medical clinic can create the biggest local impact
What does Georgia’s diabetes care shortage look like?
Georgia’s diabetes care shortage is bigger than one missed appointment or one overbooked clinic. It affects how fast people get diagnosed, how often people stay in treatment, and how many avoid serious health problems later.
As we mentioned earlier, over 1 in 10 adults in Georgia live with diagnosed diabetes. That’s over 1 million people managing this disease every day.
Even more concerning, many people do not know they’re at risk until symptoms become serious. Delayed care often leads to kidney disease, vision loss, amputations, and emergency room visits.
For healthcare providers, that creates a frustrating gap. You want prevention. Patients often arrive at crisis.
That’s where mobile clinics start to matter.
Rural Georgia feels Georgia’s diabetes care shortage the most
In places like Valdosta, Tifton, Bainbridge, and many counties across South Georgia, access is the real problem.
Some patients drive over an hour for an endocrinologist. Others skip visits because taking time off work means losing pay. For seniors, transportation can be the biggest barrier of all.
Rural counties often have higher diabetes rates and fewer healthcare resources.
That creates a cycle:
- Fewer local providers
- Fewer screenings
- Later diagnoses
- Worse long-term outcomes
A mobile health clinic helps break that cycle by bringing care closer instead of asking patients to travel farther.
Think about a county health system trying to serve five small towns with one central clinic. A mobile medical clinic can visit schools, churches, community centers, and employer parking lots. Suddenly, care feels reachable again.
And honestly, reachable care gets used.
Provider shortages make the problem worse
Georgia also faces a major provider shortage, especially in primary care and chronic disease management.
Many Georgia counties are listed as Health Professional Shortage Areas for primary care.
That means your team may already be carrying too much:
- More patients: Longer wait times for routine visits.
- Less staff: Harder follow-up for diabetes education and monitoring.
- More burnout: Providers spend more time reacting than preventing.
This is where a mobile medical unit supports your existing system instead of replacing it.
A mobile clinic van can handle screenings, A1C testing, foot checks, blood pressure monitoring, and diabetes education in the field. Your main clinic can stay focused on higher-acuity care.
That’s a smarter use of limited resources.
Diabetes care gaps also hit children and families
Georgia’s diabetes care shortage also affects younger patients.
Childhood obesity and Type 2 diabetes risk continue to rise, especially in lower-income communities with limited access to healthy food and regular care. A mobile pediatric clinic can help schools and family health programs catch warning signs earlier.
Simple mobile health screening programs can make a huge difference:
- Blood sugar checks
- Blood pressure monitoring
- Nutrition education
- Family follow-up visits
A mobile healthcare unit gives providers more chances to meet families before problems grow.
Because when care shows up in the parking lot, people are far more likely to open the door.
That leads to the next question: if the problem is this large, how exactly can mobile clinics help solve it?
How do mobile clinics help close diabetes care gaps?
When Georgia’s diabetes care shortage comes down to distance, long wait times, and limited access, the answer often starts with one simple idea: bring care closer.
That’s exactly what mobile clinics do.
Instead of asking someone in rural South Georgia to drive 90 minutes to Macon, Albany, or Savannah for diabetes care, a mobile clinic brings healthcare right to their town.
It can park at a school, church, community center, workplace, or local event.
That changes everything.
For diabetes care, regular visits matter. People need blood sugar checks, education, medication reviews, and follow-up support. When transportation becomes the problem, those visits get skipped.
Then small health issues turn into big emergencies.
A mobile health clinic helps stop that before it happens.
A mobile clinic brings diabetes care where patients already are
Mobile medical clinics work like a doctor’s office on wheels.
Your team goes to the patient instead of waiting for the patient to come to you.
That could mean:
- Visiting small towns outside Valdosta
- Parking near senior housing in Columbus
- Running school visits with a mobile pediatric clinic
- Supporting farm workers during busy harvest seasons
- Offering walk-in mobile health screening at local fairs and church events
This matters because most patients are not skipping care because they do not care.
They are choosing between:
- Gas money
- Missing work
- Childcare
- A doctor’s appointment
That’s a hard choice.
A mobile clinic helps remove that choice.
Picture someone living outside Tifton who needs regular A1C testing. The nearest provider is over an hour away. Every visit gets pushed back because life gets busy.
Then blood sugar rises. Symptoms get worse. The emergency room becomes the next stop.
A mobile medical van helps catch that much earlier.
Sometimes prevention looks less like a hospital and more like a van parked beside the local grocery store.
That’s where trust starts.
A mobile medical clinic helps with prevention and follow-up

Diabetes care is not one appointment.
It’s ongoing.
People need routine screenings, check-ins, and education over time. A mobile clinic van helps your team handle both prevention and follow-up without putting more pressure on your main clinic.
Inside a mobile medical clinic, providers can offer:
- Blood sugar testing
- Blood pressure checks
- A1C monitoring
- Nutrition counseling
- Medication reviews
- Diabetes education
- Routine follow-up visits
This is where the setup matters.
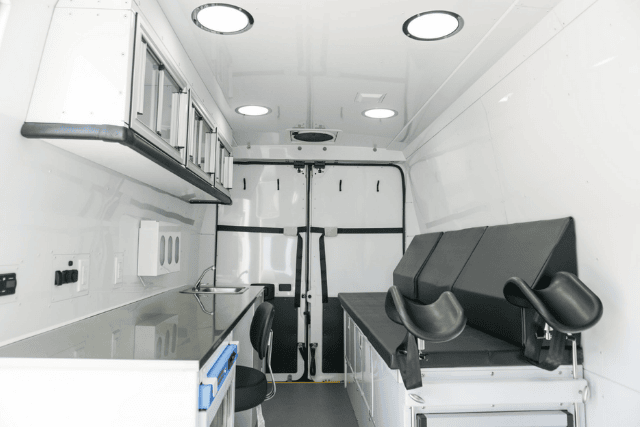
A patient bed with under-bed storage gives providers a proper place for exams and conversations. A diagnostic set helps complete important checks on-site, instead of sending patients somewhere else and hoping they actually go.
And let’s be honest, “please book that somewhere else” often turns into “that never happened.”
A sink helps with hygiene and infection control. A fridge can store medications or supplies safely.
These features make mobile medical care feel like real care, because it is.
Comfort helps people come back

This part gets overlooked.
If patients do not feel comfortable, they often do not return.
Georgia summers are hot. Really hot.
A mobile healthcare unit with rear heat and air conditioning keeps the space calm and comfortable, even during the July heat in South Georgia or chilly winter mornings.
That matters more than people think.
Nobody wants to talk about blood sugar while sweating through their shirts.
Other helpful features include:
- Privacy curtains for personal conversations
- An awning for shade during outdoor check-in
- Speakers for community education events
- Skylights that make the clinic feel brighter and less closed in
A clean, comfortable environment helps patients feel respected.
And people return to places where they feel respected.
That’s a big deal in diabetes care, where trust and routine matter so much.
A two-room mobile clinic boosts privacy
A two-room mobile clinic gives your team better flow and gives patients more comfort.
One room can be used for:
- Intake
- Education
- Family conversations
The second room can be used for:
- Exams
- Screenings
- Provider visits
This setup works especially well for:
- School health systems
- Community health organizations
A foldaway desk gives staff space for paperwork and patient education. Floor-to-ceiling cabinetry keeps supplies organized, so your team spends less time searching and more time helping.
A portable toilet can also be helpful during long outreach days in remote areas where nearby buildings are limited.
Sometimes the small details make the biggest difference.
Technology helps mobile healthcare stay connected
A mobile health unit should feel connected to your main healthcare system, not separate from it.
That’s where technology matters.
Starlink Wi-Fi helps providers access patient records, update charts, schedule follow-ups, and even support telehealth visits in rural areas where internet service is unreliable.
That’s a big deal in Georgia.
Many rural counties still have limited broadband access. A mobile health vehicle with reliable internet helps patients connect with specialists without another long drive.
Imagine doing a diabetes screening locally, then meeting with an endocrinologist through telehealth inside the same mobile clinic.
That saves time.
It saves money.
And honestly, it saves people from giving up halfway through the process.
Power supply systems also keep everything running smoothly, from laptops to refrigeration to medical equipment.
Because “the Wi-Fi stopped working” should never be the reason someone misses care.
Accessibility helps care reach everyone
Diabetes care has to work for everyone.
That includes older adults, people with disabilities, and patients with mobility challenges.
Wheelchair access helps patients enter the mobile medical clinic safely and comfortably. For seniors or patients dealing with amputations and other diabetes-related complications, that matters a lot.
Accessibility should be expected, not treated like a bonus.
A mobile healthcare vehicle built for access helps you serve the whole community, not just the easiest patients to reach.
Because healthcare should meet people where they are.
Mobile clinics help you build access
A mobile clinic does not replace your main facility.
It strengthens it.
Your main clinic can stay focused on higher-acuity care while your mobile medical unit handles outreach, screenings, education, and follow-up care in the field.
That helps your staff work smarter and helps patients get care sooner.
For Georgia organizations facing diabetes care shortages, this is bigger than buying a van.
It is about building access, helping someone catch a problem before it becomes life-changing, and turning healthcare from something hard to reach into something people can actually trust and use.
That’s where real change starts.
Next, it helps to look at which Georgia organizations benefit most from investing in a mobile clinic.
Which Georgia organizations benefit most from a mobile clinic?
The short answer? Probably more than you think.
Georgia’s diabetes care shortage affects hospitals, FQHCs, school systems, county health departments, tribal health programs, and even employers trying to support their workforce.
If your organization serves people who face barriers to regular care, a mobile clinic can help.
The goal is simple: bring mobile healthcare closer, faster, and with fewer roadblocks.
Let’s look at where mobile clinics often make the biggest impact.
FQHCs and community health centers
Federally Qualified Health Centers across Georgia are often on the front lines of diabetes care.
You are managing high patient volumes, limited provider availability, and communities where transportation is often the biggest reason patients miss appointments.
A mobile medical clinic helps extend your reach without needing to build another permanent site.
You can use a mobile clinic van for:
- Diabetes screenings
- Blood pressure and A1C checks
- Follow-up appointments
- Nutrition counseling
- Community outreach events
Instead of asking patients to travel into the clinic, your mobile health clinic can meet them where they already are.
That improves attendance and helps patients stay connected to care.
Rural hospitals and health systems
Hospitals in smaller communities often carry a heavy load with fewer resources.
Patients arrive later in the disease process because early care was too far away, too expensive, or too hard to schedule.
That turns preventable diabetes care into emergency care.
A mobile medical unit helps shift that.
Your team can use mobile medical services for outreach clinics, chronic disease management, and preventive care across nearby counties.
For example, a hospital near Thomasville could use a mobile medical van to support surrounding rural communities without asking every patient to drive into the city.
That means fewer delayed diagnoses and better long-term outcomes.
And fewer “we wish we had caught this sooner” conversations.
School systems and pediatric health programs
Diabetes care isn’t only an adult issue.
A mobile pediatric clinic helps schools and family health programs respond earlier.
Simple mobile health screening visits can identify warning signs before they become bigger problems.
This could include:
- Blood pressure checks
- Nutrition education
- Wellness visits
- Family referrals for follow-up care
A mobile health unit also makes healthcare feel less intimidating for children and families.
Sometimes a visit in the school parking lot feels much easier than missing work for an appointment across town.
That convenience matters.
Tribal health programs and community outreach teams
Many tribal and community-based healthcare programs already understand the value of meeting people where they are.
A mobile healthcare unit helps support that mission.
For diabetes care, trust matters just as much as access. Patients are more likely to engage when care feels familiar and local.
A mobile health van with clear community branding parked at a trusted gathering place can make a huge difference.
It helps with:
- Regular screenings
- Medication support
- Follow-up visits
- Health education
- Telehealth access through Starlink Wi-Fi
This creates stronger relationships, not just faster appointments.
And stronger relationships lead to better health outcomes.
Employers and workforce health programs
This one surprises people.
Large employers, especially in agriculture, manufacturing, and logistics, can also benefit from mobile healthcare vehicles.
Workers managing diabetes often delay care because missing a shift means losing income.
A mobile clinic parked on-site makes care easier to access without creating another burden.
That helps with:
- Preventive screenings
- Blood pressure checks
- Diabetes education
- Early referrals for treatment
Healthy employees mean stronger operations, fewer emergency absences, and better long-term workforce health.
Sometimes the best healthcare strategy starts in the employee parking lot.
The real question is access
The better question isn’t “Who needs a mobile clinic?”
It’s “Where are people falling through the cracks?”
That’s where a mobile medical vehicle creates the most value.
If patients are missing care because of distance, transportation, scheduling, or trust, mobile clinics help close that gap.
And when you close that gap, you’re doing more than improving healthcare access.
You are helping people stay healthier, longer, protecting dignity, and saving lives.
That’s the real job.
Ready to solve Georgia’s diabetes care shortage with a mobile clinic?
You came here because Georgia’s diabetes care shortage is creating real pressure for your organization. Patients are missing care, providers are stretched thin, and the gap between people and treatment keeps getting wider.
Now you know that the gap can be closed.
Here’s what we covered:
- Georgia’s diabetes care shortage is driven by distance, provider shortages, and delayed preventive care
- Mobile clinics bring mobile healthcare directly into rural communities, schools, workplaces, and trusted local spaces
- A mobile medical unit helps improve screenings, follow-up care, education, and long-term patient outcomes
At AVAN Mobility, we work with healthcare organizations that are trying to solve real access problems, not simply add another vehicle to their fleet. From rural health systems to FQHCs and tribal health programs, we help teams design mobile medical clinics around how care actually happens in the field. Every mobile clinic we build is focused on reliability, patient dignity, and making healthcare easier to reach for the people counting on you most. That’s why we lead with conversations first, not sales pitches.
Because at the end of the day, this work is about people. It is about helping someone get care before a small issue becomes a life-changing one. If you have questions, click the button below to talk to a mobility expert who understands the road you are on.
If you’re not ready to talk to a mobility expert yet, we have a few other resources you should check out to learn more.
Recommended next reads
- How much does a mobile medical unit cost in the U.S.? Cost is usually the next big question, and this article helps you understand pricing, budgeting, and what affects your investment.
- A guide on securing grants for mobile health clinics in the U.S.: If funding is part of your planning, this article walks through where organizations find grants and how to improve your chances of approval.
- How to choose a mobile medical van: Once you know mobile care is the right move, this helps you compare options and understand what features matter most for your program.




